Our Immune Recovery & Resilience Programs
The immune system is designed to protect and adapt, but when it becomes chronically activated or dysregulated, it can contribute to persistent symptoms that affect energy, cognition, digestion, mood, and overall resilience. These patterns may arise following infections, environmental exposures, autoimmune activity, or prolonged physiological stress. Our programs are based in functional medicine, use integrative therapies for support and are uniquely guided by neuroscience data and interventions to assist the body in both repair and resilience by connecting brain function to all systems affected by illness and disease.
Immune & Auto-Immune Disorders
Autoimmune and immune-related conditions often reflect a loss of immune regulation rather than a single isolated problem. When the immune system remains overactive or misdirected, it can contribute to chronic inflammation, fatigue, pain, cognitive changes, and multi-system symptoms that are difficult to resolve with symptom-based care alone.
Our Autoimmune & Immune Support program focuses on understanding why immune balance has been disrupted and how it interacts with metabolism, stress physiology, the nervous system, and environmental factors. Care is individualized and paced, with attention to reducing unnecessary immune activation while supporting resilience and adaptation over time.
This program may be appropriate for individuals managing autoimmune conditions, chronic inflammatory symptoms, post-infectious immune changes, or ongoing immune dysregulation without clear answers.
Biotoxin & Mold Illness
Certain individuals are more susceptible to environmental and biological stressors that can disrupt immune regulation. When exposure to biotoxins, infections, or environmental triggers overwhelms the body’s adaptive capacity, immune responses may become persistently activated rather than self-limiting.
Conditions such as Chronic Inflammatory Response Syndrome (CIRS) and Mast Cell Activation Syndrome (MCAS) reflect patterns of immune dysregulation in which the body reacts excessively or inappropriately to otherwise manageable stimuli. These responses may be triggered by factors such as water-damaged buildings, mold or fungal exposure, tick-borne illness, environmental chemicals, or certain medications.
Rather than focusing on exposure alone, our approach evaluates how immune activation, inflammation, nervous system signaling, and metabolic stress interact — and how these systems can be supported toward improved regulation and resilience.
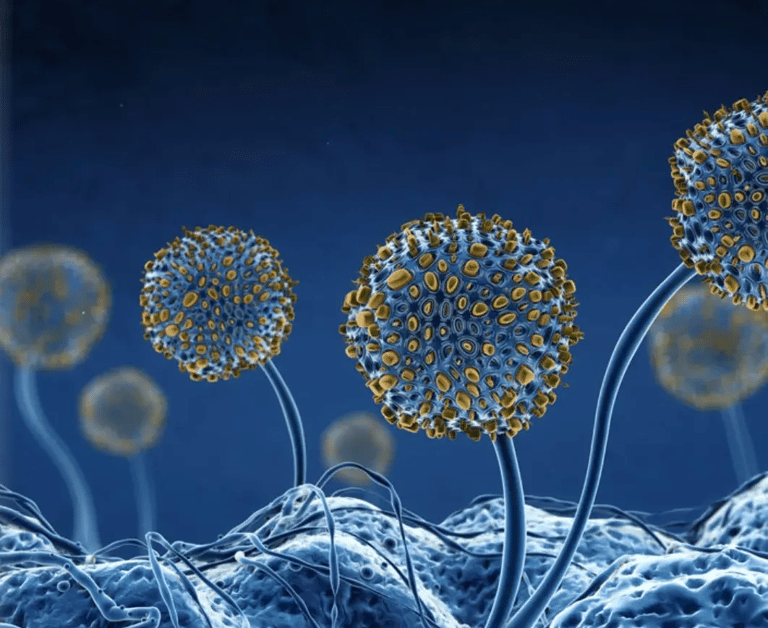
Tick-Borne Illnesses | Co-Infections
Lyme disease is a multi-system bacterial infection caused by the spirochete, Borrelia burgdorferi, which is transmitted to humans primarily through the bite of an infected deer tick. Lyme disease has several different stages: first stage (acute/early localized), second stage (early disseminated), and third stage (chronic/late disseminated). Symptoms vary depending on the stage of illness. In early Lyme disease, patients can present with a rash and/or flu-like symptoms. In later stages symptoms can manifest in multiple body systems, including musculoskeletal, heart, brain, and nervous system.
What is the treatment for Lyme Disease?
The first-line standard of care treatment for adults with Lyme disease is doxycycline, a tetracycline antibiotic. Other antibiotics that have activity against borrelia include the penicillin-like antibiotic, amoxicillin, and the second generation cephalosporin, Ceftin. The mainstay of treatment is with oral (pill) antibiotics, but intravenous antibiotics are sometimes indicated for more difficult to treat cases of neurologic-Lyme disease, such as meningitis, and cases of late Lyme arthritis. Additional therapies at our facility can include IV therapies, Herbal medicines and supplements which can support individualized programs.
Adaptive Immune Resilience
Some immune-related conditions do not fit neatly into traditional autoimmune or infectious categories. Instead, they reflect patterns of immune dysregulation — where the immune system remains overly reactive, poorly regulated, or unable to return to baseline after stress, infection, exposure, or medication use.
The Adaptive Immune Resilience Program is designed for individuals experiencing complex immune-mediated patterns such as mast cell activation (MCAS), chronic inflammatory response patterns (CIRS), fluoroquinolone-associated dysfunction (FQAD), and post-viral or post-infectious syndromes, including those following COVID-19.
These conditions often require a different clinical strategy than standard immune suppression or symptom-based care. Our approach focuses on understanding how immune signaling, nervous system regulation, metabolism, and environmental stressors interact — and how to support adaptive recovery over time.
Care is individualized, paced, and responsive, with the goal of reducing unnecessary immune activation, improving tolerance, and restoring functional resilience rather than chasing isolated triggers
Many immune-related conditions overlap across categories. What matters most is how the immune system is behaving, not just the name of a condition. This is why care is individualized and why different immune patterns require different clinical strategies.